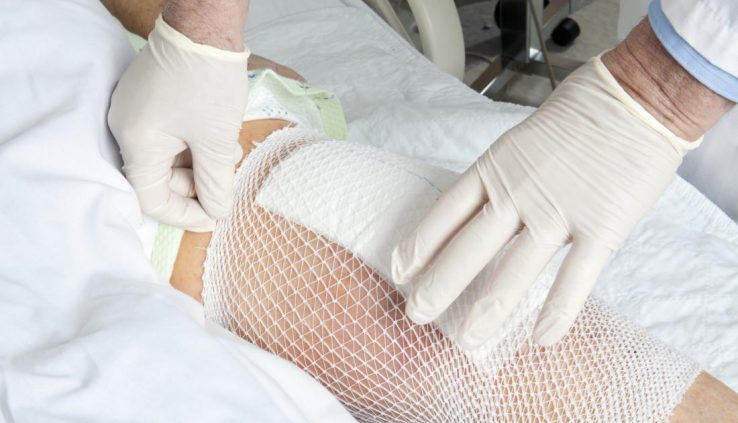
Infection after total knee replacement
Contents:
- Early and deep total knee infection
- Risks for total knee infection
- Diagnosis of total knee infection
- Prevention of total knee infection
When does the total knee infection occurs
The classification is important because it has bearing on the outcome of the treatment of total joint infections. You have much better chances to get your total knee infection healed if it appeared early and was treated promptly.
Early postoperative total knee infection
appears within one month after the operation
Late infection
appears later than one month after the operation. The majority of the late chronic infection develops months or even years after the operation. Many of the patients with late infections around the total knee joints were never completely pain-free; some patients developed sinuses, draining holes in their operation wounds.
Two thirds of all total knee infections appear three months or later after the surgery. (Peersman 2001)
The signs of an early PWI
Basically, this is infection of the hematoma (collection of blood) that assembled in the wound after the operation.
The patient runs high temperature and has severe pain from the whole knee joint. The operation wounds is painful, red,occasionally with pus running from it. The whole knee joint is swollen. Because of such dramatic signs, the early total knee infection is discovered and treated promptly, before the bacteria have had time to settle down on the total knee prosthesis.
Treatment is always operative: The surgeon opens the operation wound, evacuates the infected hematoma, lavages (flush) the wound with antibiotics. Massive antibiotic treatment follows. Usually, the fixation of the total knee joint to the skeleton is good so that the total knee joint is retained.
With quick treatment the majority of the early total knee infections will heal without further consequences for the total joint.
The signs of a late PWI
The infection develops late, months or years after the patient left the hospital with the operation wound healed. The patient notices increasing pain in the operated knee joint, the pain is worse when the patient puts weight on the knee. The knee joint is swollen and stiff. In some patients there develops also openings in the operation wound that a secret pus-like liquid.
The blood tests show elevated parameters for ongoing infection and the temperature might be slightly elevated. In the minority of patients the late deep postoperative infection may be so stealthy that even the infection parameters may be at the borderline to the normal.
Because the late PWI develops so stealthily during a long time, the bacteria have had ample time to destroy the bone stock to which the total knee joint was once anchored. Therefore, the treatment of the late total knee infection is difficult and the results are less predictable.
Acute hematogenous infections
It is a special and rare form of the infection around the total joints. It occurs at once in a previously well functioning total knee joints, years after the operation.
It is caused by bacteria from a remote infection that traveled through the blood stream and get stuck on the surface of the total knee joint. There the bacteria are inaccessible to the body’s defense system and may develop a rather widespread infection.
Occasionally, there is an obvious source of infectious bacteria (skin boil, infected tooth, leg wound, e.g) elsewhere in the body, but not always.
The total knee joints are most susceptible to this rare form of the joint infection during the first two postoperative years. The risk of the acute haematogenous total knee infection makes that you should take a dose prophylactic antibiotic every time before procedures that may push bacteria into the blood circulation. See also the chapter Antibiotic treatment.
The treatment of this special infection form of infection is by operation.
If the infection has been discovered and treated early, the results of treatment of haematogenous total joints infections are equally good as treatment of early total joints infections.
For more details about the treatment of total knee infections see the chapter Treatment of total knee infections.
How frequent are the infections around a total knee joint?
The deep PWI after total knee surgery are rare nowadays, only about 0,3 to 0,5% of primary total joint operations develop deep PWI. Moreover, the risk of total joint infection diminishes as the surgeons develop new methods how to prevent total joint infection.
Risk factors for development of deep PWI are:
Previous operation in the knee joint increases twice the risk of postoperative infection.<
| Operation | Per cent infections |
| first operation | 0,4 % |
| second (revision) operation | 1,0 % |
The risk of total knee infection is even higher in patients with previous infection in the operation area.
Other factors such as diabetes, obesity, rheumatoid arthritis, immune- suppressive treatment, and history of smoking also increase the risk of total knee infection.
What is not a PWI:
- a redness of the skin around the operation wound without swelling or pain,
- a slight swelling with blue discoloration of the skin around the operation wound
- small areas of the operation wound that are black
- a drop of clear fluid that appears around the stitches of an uneventfully healing operation wound
- a positive bacterial culture from such liquid that shows growth of skin bacteria.
With proper care of the operation wound, changes of dressing and removal of stitches if necessary, these disturbances in the healing of the operative wound resolve themselves and they are nothing to worry about.
Superficial postoperative wound infection
Collection of blood (haematoma) beneath the skin may occasionally become infected. This is a superficial postoperative wound infection. The signs are pain, redness, swelling of the operative wound. This complication must be treated acutely (operative evacuation of the infected hematoma)
The total knee joint is positioned quite superficially and lacks effective protection against the spread of the superficial infection into the deeper total knee. Thus it is important that the surgeon evacuates the infected haematoma promptly. After such treatment the superficial postoperative wound infection usually heals without further complications.
Tests to diagnose a total knee infection
(See also the chapter: Diagnosis of the knee disease)
Blood tests:
- ESR – elevated
- CRP – elevated
- WBC – white blood cells count – elevated rarely
X-rays : generally there is destruction of skeleton around the infected total joint prosthesis. The surgeon accordingly suspects total knee infection every time when the X-ray picture shows widespread destruction of the skeleton around the prosthesis. But there is no specific X-ray picture pinpointing to the total knee infection.
Other diagnostic methods to arrive at the diagnosis of total knee infection:
Gallium and Indium bone scans
Puncture, aspiration, and bacteriological culture of the total knee joint. The surgeon uses a long injection needle on a syringe and sucks the joint fluid. Examination is done under sterile conditions
Reliability of this methods depends on the bacteriological technique used for growing the bacteria. If identical bacteria grow in several samples, the infection if proven, but absence of bacterial growth does not exclude the infection!
Direct microscopic examination of the tissues during the revision operation
Bacteriological culture from the tissues removed during the revision operation
The bacteriologists have developed also a very sensitive “molecular diagnostic method” to identify the presence of any bacteria in the operation wound. The method, the polymerase chain reaction, can trace small amounts of bacterial DNA. The disadvantage of this method is that it may detect the presence of bacteria that are not causing any infection.
Nothing grows from the sample taken from my operation wound, but I still have an infection
Up to 20 % of obviously infected total knee replacements had no bacterial organisms that could be identified. Why?
Some bacteria are slow “growers”.
The main reasons why nothing grows from the samples taken from an obviously infected total knee, however, are:
- bacteria afherent to infected total knee device will not grow. other methods for identification are necessary, see the chapter: Bacteria NonGrowth Identification
- faulty bacteriological technique (anaerobe bacteria need special cultures)
- long antibiotic treatment before the sample was taken (all antibiotic treatment should be stopped for some weeks before taking samples for bacterial cultures).
- few samples taken (at least seven samples should be taken during a revision operation and be sent for culture).
Prophylaxis against postoperative wound infection
“With improvement of technology in clean air theatres, and availability in practice, slackness has crept into (operation) theatre protocol.”
Medhavan 1999
Prevention at operation
The absolute majority of the total hip infections is caused by bacteria that landed in the operation wound during the total hip joint surgery from the air. The surgeon, his operation team, and the patient are spreading these bacteria continually from the surfaces of their bodies into the air.
Clothes
The source of all bacteria on an operation room are people working there AND the patient. The bacteria are produced on the body surface (mainly groin, inside of the thigh, and arm-pitts and travel on tiny skin scales in the air of the operation room. Every healthy person produces about 1000 such bacteria bearing skin scales per minute.
ISo the surgeons (borrowing experience from atomic industry) developed impermeable, ventilated, astronaut-like gowns. The proper term is Body Exhausted Suits (BHS). The BES are made of hydrophobic materials, according to national and international standards. In spite of advertizing, these BES are uncomfortable, awkward to work in and expensive.
Several studies demonstrated that modern occlusive clothing is equally effective as body exhaust suits to diminish the counts of bacteria in the operation room air. Moreover, it is more agreable to work in and much cheaper.
Ventilation of the operation room
Operation rooms are placed in the hospitals. The air on the hospital wards is dirty with hospital bacteria, sailing on the skin scales. If such ward air penetrates into the operation room, the dangerous hospital bacteria will settle into the operation wound.
So the surgeons constructed laminar air ventilation systems for the operation rooms. Such ventilation systems produce huge volumes of a very clean air so that the whole volume of the air in the operation room changes 300 -500 times per hour.
The use of sterile operation rooms and astronaut -like operation gowns diminished the risk of postoperative infection from previous 2-3 % to 0,2-05%.
Prophylactic antibiotics
In modern total joint surgery, practically all total joint operation patients, either operated on super-sterile or conventional modern operation rooms will get prophylactic antibiotic.
Moreover, many patients will get prophylactic antibiotics in bone cement too . Studies demonstrated that these patients will have still lower rates of postoperative infections.
For more information see the chapter Prophylactic antibiotics
What you can do yourself
- Avoid skin damage and open wounds in the legs
- Treat every infection anywhere in the body
The rate of infections in individual hospitals
The rate of PWI after total hip and knee operations varies among individual hospitals.
Small variations of these low rates of PWI are caused by factors that are beyond the control of the surgeon. For example, if the hospital operates on many difficult cases, with long operation times, there would be higher rates of postoperative infection. If the rates of postoperative infections rise to the 1% level or above it, however, the surgeon should be concerned and make a close check-up of hygienic routines on the operation room.
Studies demonstrate that the rate of postoperative infections is higher after total hip operations done in hospitals with low operation volume by the surgeons who carry out total hip replacement only seldom. (Katz 2001). Available statistics confirm that this observation applies for total knees too.
The only way for you to know how many postoperative infections there have been in the hospital you choose for your operation is to ask directly. All hospitals should keep reliable statistics about the rates of postoperative infections occurring after the operations done on their operation rooms. As a collateral, you may ask about the annual volume of total joint operations.
If the surgeons in the hospital perform less than ten total hip or knee operations per year then the risk of postoperative infection in such a hospital may be higher then average.
Wish to know more facts about
| treatment of infection with antibiotics |
References:
- Katz et al J Bone Joint Surg-Am 2001: 83-A:1622 -29
- Medhavan et al Deterioration of theatre discipline during total joint replacement. Ann R Coll Surg Engl 1999; 81: 262-5
- Peersman G et al Clin Orthop 2001;392:15 – 23
- Spangehl A. J Bone Joint Surg-Am, 1999;81-A:672-83