What is a total knee prosthesis
Contents:
classification of total knee prostheses
posterior stabilized total knee
cemented / cementless total knee
materials for total knee / incongruent joint surfaces
There is no such total knee joint prosthesis that can mimic the complicated forms of surfaces of the knee joint and the “fuzzy biomechanics” of a healthy knee joint. Every total knee joint prosthesis is thus a compromise, that mimic only certain characteristics of the natural knee joint. The classification of total knee prostheses is equally “fuzzy”.
Classification of Total Knee Prostheses
Here follows an arbitrary classification of total knee prostheses. This classification is based on:
- How much of the joint surface is replaced
unicompartmental and tricompartmental TKP - Posterior cruciate ligament (PCL) state
PCL retained and PCL removed (” posterior stabilized”) TKP - Mobility of the polyethylene joint surface (bearing)
fixed polyethylene (PE) bearing and mobile PE bearing TKP
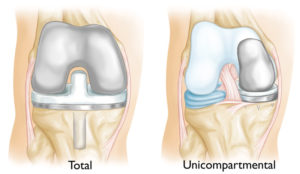
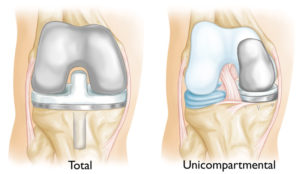
Unicompartmental and tricompartmental TKP
The normal knee joint has three chambers -compartments.
According to how many of the three knee joint compartments will be replaced with the kne joint device There are two models of total knee prostheses, the one model replaces only one compartment of the knee joint, the other model replaces the whole (or almost) knee joint.
Unicompartmental total knee prosthesis:
Unicompartmental knee prostheses provide for replacement of only one knee joint compartment, i.e. the opposing joint surfaces of the femur and tibia, either on the inside or on the outside of the knee joint.
In other words, this is only a partial knee joint replacement.
Tricompartmental total knee prosthesis:
provides for replacement of all three knee joint compartments (spaces), that is the replacement of whole joint surfaces of femur, tibia, and patella. This is a true total knee replacement.
The names of the total knee prostheses are long tongue-breaking creations. Savor this combination in the title of a paper: “Use of unicompartmental instead of tricompartmental prostheses for unicompartmental arthrosis in the knee…”.
Description of the Unicompartmental knee prosthesis
Unicompartmental knee prosthesis is used in knees where only one half (one compartment) of the joint is affected by the disease. In this picture the medial compartment (inner part) of the knee joint has been replaced.
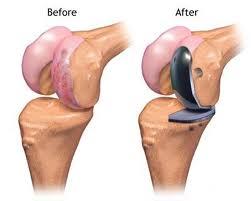
The unicompartmental knee prosthesis has two components. The femoral component which replaces the joint surface of the femoral condyle is a bent metallic plate with a slightly convex joint surface. The curvature of the bent plate imitates the curvature of the natural femoral condyle.
The tibial component which replaces the tibial joint surface is an almost flat tibial plate which has semicircular surface and is fabricated from polyethylene. The polyethylene plate has often metal backing made from titanium.
The polyethylene plate is either fixed to the metal backing plate by the manufacturer or it moves freely on the polished surface of the metal backing envelope.
This later model is also called menisceal bearing unicondylar prosthesis. The polyethylene plate mimics the function of the meniscus in the healthy knee because it glides forwards and backwards on the polished plate during extension and flexion of the knee joint as does the natural meniscus.
Both components have pegs for better fixation to the skeleton.
Description of Tricompartmental total knee prosthesis
Tricompartmental total knee prostheses provide for replacement of all three knee joint surfaces, including the patellar surface.
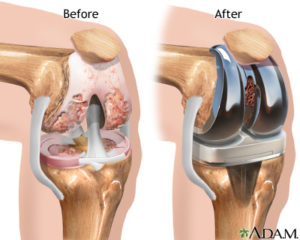
The surgeon, however, may decide not to replace the patellar surface.
The convex femoral component of a total knee prosthesis is a large plate bent to accommodate the curvatures of the femoral condyles. The femoral component has a large flange in front for contact with gliding patella.
The slightly concave tibial component is a plate made of a UHMW (ultra high molecular weight) polyethylene. The plate is often enclosed in a metallic retainer (back-up). The metallic back-up helps to minimize the deformation of the polyethylene component under loads. The metallic back-up is often fabricated from Titanium.
Also the patellar component (made of polyethylene) may have a metallic back-up.
The surfaces of the total knee components in contact with skeleton are provided with pegs that improve the fixation of the components to the skeleton.
(the picture shows Genesis total knee, Smith&Nephew)
Posterior stabilized and PCL retained total knee
Posterior cruciate ligament (PCL) is an important structure that stabilizes the knee joint. In knee joints with severe osteoarthritis, this ligament is, however, often defective or absent.
Many surgeons believe that when the PCL is well functioning, it should be retained during the total knee replacement. For this purpose there are available PCL retaining Total knee prostheses.
Other surgeons believe that PCL cannot function well in a total knee prosthesis and should be always removed before the total knee is implanted. These surgeons also believe that after removal of the PCL the surgeon should implant a special total knee prosthesis that simulates the function of the PCL.
There are thus available special posterior stabilized total knee prostheses for operation of knee joints without PCL
The stabilization of the total knee joint in these prostheses is achieved by a clever “cam and post” mechanism added to the prosthesis components. This mechanism replaces the function of the PCL.
For more information on these models see the chapter Posterior stabilized TK
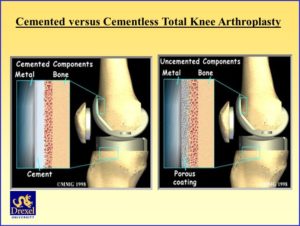
Cemented OR Cementless TKP
Everyone of these prostheses may be fixed to the skeleton
- without bone cement – cementless total knee prostheses, press fit fixation
- or with bone cement cemented total knee prostheses.
The cementless total knee prosthesis
The surgeon pushes (blows, hammers) the prosthesis directly on the raw bone surfaces. The prosthesis is held in place by the elasticity of the bone tissue and by the friction between the surfaces of the skeleton and the prosthesis.
Total knee prostheses for cementless use have often porous coatings on the surfaces that are in contact with the skeleton. The porous coating partly enhances the friction of the prosthetic surfaces against the skeleton, partly it enhances the ingrowth of the host’s bone into the porous surface
In this way the porous coating improves the early fixation of the prosthesis and it produces a lasting biologic fixation of the prosthesis to the skeleton later.
The surfaces of the total knee components in contact with skeleton are provided with stems that improve the fixation to the skeleton.
The patellar component that articulates with the metallic flange of the femoral component is also made of polyethylene, although it is convex. It has also a metallic back-up.
(The stems are extra long because this is a PCA revision prosthesis – Howmedica)
The cemented total knee prosthesis:
The surgeon puts a thin layer of bone cement between the prosthetic components and the prepared skeleton surfaces. It depends on the surgeon if he uses the bone cement for fixation for all components of the total knee joint or if he/she uses the bone cement for fixation of only some components.
When the self curing bone cement hardens, it fixes firmly the total knee components to the skeleton.
The advantages of bone cement fixation:
The layer of bone cement will level off all unevenness of the cuts made in the skeleton.
The cement layer acts as an intermediate bumper between the very stiff metal of the components and the relatively soft skeleton.
The bone cement seals the interface between the prosthesis and the skeleton. The joint fluid with polyethylene wear particles cannot enter this space and provoke osteolysis
The disadvantages of bone cement fixation
Pressing the doughy bone cement into the marrow cavity of the thigh and shin bones may cause general circulatory disturbances
The bone cement layer ages, cracks, and after some time the bond between the prosthesis and the skeleton is lost .
The advantage of cementless fixation
Absence of small particles of hard bone cement that occur between the total knee surfaces and increase polyethylene wear
The disadvantage of cementless fixation
Absence of seal of the space between the total knee prosthesis and the skeleton. In many statistics, cementless total knees demonstrated higher rates of loosening than the cemented prostheses.
Mobile and fixed bearing of polyethylene joint surface
In the conventional total knee prosthesis the polyethylene component is flat and fixed to the tibia (shinbone). This construction is called fixed (stabile) bearing total knee model
In the natural knee joint, the joint surfaces between tibia and femur are not conforming. Nature has placed a piece of triangular cartilage between these two joint surface, the meniscus, which takes up and distributes the stresses evenly between the tibial and femoral joint condyles.
The menisci in the natural knee move quite a lot, and the clever surgeons who discovered this fact put a moving piece of polyethylene to replicate the Nature’s moving interface system in their total knee joint prostheses.
Such a total knee model is called mobile bearing total knee joint.
For more information on this model see the chapter Mobile bearing TK
MATERIALS FOR TOTAL KNEE PROSTHESES
IMPORTANCE OF CONGRUENCY
In total knee prostheses the form dictates the choice of materials for the joint surfaces of the prosthesis.
In congruent ball and socket joints, such as the hip joint, the stress is distributed evenly. Such artificial joint may have joint surfaces of hard materials, such as ceramic or metal.
In incongruent (not concentric) joints, such as the knee joint, contact of two incongruent hard surfaces creates very high peak stresses. The hard surface material, especially ceramic, cannot sustain such peak stresses and wears off.
This is the reason why the choice of materials for the joint surfaces of a total knee joint prosthesis is limited.
Total knee prostheses usually have a metallic femoral component, fabricated from modern Cobalt- Chrome alloys and a tibial component made from Ultra High Molecular Weight PolyEthylene (UHMWPE).
The polyethylene component is often metal-backed.
Combinations of two hard joint surfaces such as metal on metal and ceramic on ceramic are not used in construction of total knee joints, because they wear too much when subjected to high stresses.
According to one report, however, there are laboratory experiments underway to produce a new model of ball and socket total knee prosthesis that may avoid the polyethylene altogether. (Heimke, 2002)
The concern for polyethylene wear has, however, led to the development of ceramic-on-polyethylene total knee prosthesis models. The convex femoral component of these prostheses is made of ceramic, the tibial component is the conventional polyethylene plate. These models are not in general use on the European continent and in the USA.
One Japanese total knee prosthesis (The bisurface total knee, Akagi 2001) uses alumina ceramic, the other one ( Oxinium, Smith&Nephew) uses oxidized Zirconium.
Theoretically and in laboratory experiments, the wear of the bearing combination zirconium oxide on polyethylene is much lower than the wear of the bearing combination Cobalt-Chrome on polyethylene. As yet, there are no peer reviewed reports on the oxinium total knee joint. For more information see www.oxinium.com., www.oxidizedzirconium.com .
The concern for breakage of the ceramic components in total joint prostheses apply to the ceramic-on-polyethylene total knees too, although no breakage has been observed in the Japanese bisurface total knee. The authors of that prosthesis, however, caution that the prosthesis was used in Japanese population only, which is known to have lower body weight.
References:
Heimke G et al Biomaterials 2002; 23: 1539 -51
Akagi Masao A, et al. J Bone Joint Surg-Am; 82-A: 1626-33