Diseases of the knee joint
Contents:
- Arthritis
- Osteoarthritis of the knee
- Isolated femropatellar osteoarthritis (kneecap osteoarthritis)
- Rheumatoid arthritis
- Lupus
- Osteonecrosis of the knee
- The previously infected knee
The diseases that most frequently lead to the total knee surgery are:
- Osteoarthritis (primary and following after knee damages) = ca 80%
- Rheumatoid arthritis = ca 15%
- Conditions after fractures of the knee joint= ca 4%
The spectrum of diagnoses that lead to total knee surgery varies with the age of the patients:
- in young patients prevails rheumatoid arthritis and reststate after joint trauma
- in older patients prevails osteoarthritis and osteonecrosis of the knee joint
Arthritis
the term literally means inflammation of the joint (arthritis is Greek for joint inflammation). But the English language usually uses this term to describe any condition in which there is a damage to the joint, even in cases where the inflammation is absent.
It is important to distinguish between
- osteoarthritis which is a strictly local cartilage damage in one joint not caused by inflammation
- rheumatoid arthritis which is a serious systemic disease, affecting many joints and other organs as well, and accompanied by severe inflammation.
Osteoarthritis of the knee joint (O.A.)
Surgeons distinguish two forms of osteoarthritis
- the idiopathic OA – as the name idiopathic says, no one knows for sure what causes the destruction of the joint cartilage
- the secondary OA – the damage to the cartilage in the knee joint has a known cause such as previous fracture through the joint surfaces or damage to the meniscus or ligaments of the knee joint.
The joint cartilage layer in osteoarthritis becomes thinner and eventually disappears entirely so that only raw bone ends come in contact with each other. The grating of raw bone ends in direct contact causes pain and stiffness in the knee joint.
The contours of the bone ends enlarge and bone spurs forms at the periphery of the knee joint.
Joint capsule enlarges and becomes thicker. The quantity of joint fluid increases (effusion). Distended joint capsule makes the movements in the knee joint painful.
Small fragments of damaged joint cartilage float in the joint fluid and cause secondary inflammation of the synovium (the inner lining of the joint space) with swelling and pain in the knee joint.
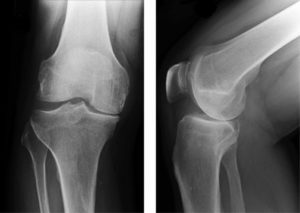
The joint cartilage damage may be restricted only to one knee joint compartment, as in this picture, or the whole knee joint may be affected by osteoarthritic changes.
In knee joints with changes restricted to only one knee joint compartment, it is most often the inner (medial) compartment that is damaged by OA, whereas other compartments may have still healthy cartilage. In this picture the outer (lateral) compartment has healthy joint cartilage and meniscus.
Note also, that the axis going through the knee joint is distorted
There is no blood test for OA. The laboratory tests are only necessary if your doctor will exclude other forms of arthritis (such as rheumatoid arthritis) as a cause of the knee joint damage.
Do all patients with osteoarthritis of the knee joint need an operation?
Large studies demonstrated that up to 40 % of all patients with signs of osteoarthritis of the knee joint on X-ray pictures have been satisfied with conservative treatment.
Conservative treatment comprises
Exercises, drugs, nutritional supplements (chondroitin and glucosamine), intra-articular injections (Hyaluronic acid), special unloading braces).
Operative treatment may offer a variety of operations, depending on many factors such as the patient’s age, progress of the osteoarthritis, etc.
For more information visit the chapter Alternative knee operations.
Isolated femorotellar osteoarthritis
For the anatomy of the femoropatellar joint see the chapter Total knee operation.
Cartilage in the femoropatellar joint is usually damaged by a direct trauma against this joint (dashboard trauma with car accident when the car’s dashboard collides with the front side of the knee), or
by osteoarthritis – worn out joint cartilage. This is usually caused by wrong position of the patella in the femoral groove.
Patients with damaged or worn out cartilage of the kneecap’s joint usually have severe pain in front of the knee joint. X-ray picture usually shows the cause of pain: diminished space in the femoropatellar joint and/ or changes in the position of the patella.
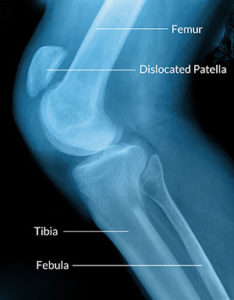
Picture: X-ray picture so called CT) demonstrating partly dislocated kneecap. Note that there is bone-bone contact between the patella and the femoral bone, i.e. the joint cartilage is totally worn out in this area. Such conditions are very painful. (Adapted from Saleh et al. J Bone Jt Surg, 2005, 87-A, 664)
In patients with the damage limited to the femoropatellar joint only, the surgeons in the past often removed the whole kneecap. The results of this operation were seldom satisfactory.
In young patients two new types of operations were introduced lately:
1) Transplantation of patient’s viable cartilage cells to replace the damaged joint cartilage. This operation has been successful in knee joint with small cartilage defects and well retained alignment of the whole joint.
2) Replacement of the damaged cartilage with an artificial joint. In young patients replacement was done with devices that replace only the femoropatellar joint.
Picture: Prosthesis that replaces only the femoropatellar joint. The results with old types of such replacements were not very good. The modern devices show as yet good results (Adapted from Saleh et al. J Bone Jt Surg, 2005, 87-A, 666).
In older patients the surgeons often recommend to carry out a total joint replacement. This operation gives excellent results in the majority of older patients patients.
Reference:
Khaled J Saleh et al: Symposium. Operative treatment of patellofemoral arthritis. J Bone Joint Surg-Am 2005; 87-A: 659-71
Rheumatoid arthritis (R.A.)
Rheumatoid Arthritis (R.A.) is a general inflammatory disease.
It comes in waves (flares and remissions). If untreated, as years pass, the inflammation becomes a norm. In addition to painful, inflamed joints, many people with R.A. feel as if they constantly “have flu”, feeling mild fever, extreme fatigue and weight loss.
The same inflammatory process that damages the joint can also affect the eyes, lungs, heart, kidneys, and blood vessels. Untreated severe R.A. has the potential to shorten the patient’s life.
It is counted to a large group of autoimmune diseases.
The joint inflammation successively destroys the joint cartilage and bone tissue. Bone tissue becomes soft, the damage to the bone tissue may be enhanced by the corticosteroids used for treatment of R.A.
On X-ray pictures the shadow of joint line is lost. But the X-ray pictures of a R.A. joint also show a striking loss of bone tissue in the skeleton around the inflamed joint. Sometimes a large parts of the bony joint surfaces are destructed by the inflamed joint tissue (synovial lining).
Blood tests: The Erythrocyte sedimentation rate is elevated. This test is, however, not specific for R.A.
Rheumatoid factor (RF), an antibody secreted by certain body’s cells, is found in the blood of up to 85 % people with R.A who have had R.A. for more than 18 months. The positivity of this test usually heralds the begin of a more aggressive phase of the disease. This test is sometimes positive in otherwise healthy people aged over 70.
The skeleton of patients with R.A. is “soft”, the marrow cavity of femoral bone is large, and these patients often have cortisone treatment also after the total knee replacement. Cortisone inhibits the formation of the new bone. These factors taken together make the use of cementless total knee prostheses in patients with R.A. problematic.
The engagement of other joints makes the R.A. patients less mobile. Thus, improvement of the function in only one knee joint after a total knee operation improves the situation of these patients considerably.
Moreover, the artificial joints of these patients are not exposed to excessive loads, so that the results of the total hip operation in these patients are surprisingly good. There is also lover risk of deep vein thrombosis in the patients with R.A.
Because R.A. is a systemic disease, many alternative knee operations such as tibial osteotomy are not feasible. Limited operations, consisting in removal of inflamed synovial tissue (synovectomy), done often on smaller joints, may be, however, useful also on the knee joint. The synovectomy removes the synovial lining of the knee joint, the big producer of detrimental enzymes that are continually damaging the knee joint cartilage. This operation may, thus, stops the deterioration of the joint
These operations are, however, producing relief only for a limited time period.
The total knee replacement operation is, on the other side, a definitive procedure that stops the progress of the disease in the operated joint.
There are, however, some increased risks for patients with R.A. who are operated on with total knee replacement.
There is an increased risk of prosthetic infection. The disease itself and the use of Corticosteroids make these patients susceptible to general infection which then engages the artificial knee joint.
There is an increased risk of fracture of the bones around the total knee joint because the skeleton is soft.
These patients often have very thin skin so that they often develop skin bruises. These bruises may be infected and be a portal for a bacterial infection.
There is engagement of other joints which are equally stiff and destructed as the knee joints. Stiff, immobile cervical spine, with soft, partly destructed vertebrae, may produce problems for anesthesia. It is important to take X-ray pictures of the cervical spine and consult the anesthesiologist before the contemplated operation.
Lupus
Lupus (whole name Systemic Lupus Erythematosus or SLE) belong to specific inflammatory diseases called also collagen diseases. These disease attack soft tissues containing collagen fibers. Lupus is a systemic disease, which often damages hands, but it may damage also large joints, mainly knees. Lupus is treated with high cortisone doses and the patients so treated often develop osteonecrosis of both hip and knee joints. In a patient with known osteonecrosis of one knee joint it is thus mandatory to evaluate and examine the hip joints too.
Because lupus is a systemic disease that damages heart, lungs, kidneys, and blood vessels, these patients must have a thorough preoperative examination and a consultation with a rheumatologist before the knee surgery could be contemplated.
Osteonecrosis of the knee
Osteonecrosis (death of the bone tissue) of the knee includes two distinct entities
- spontaneous osteonecrosis and
- atraumatic osteonecrosis
Spontaneous osteonecrosis of the knee joint
usually affects y people after 60 years of age. The only sign is often a sudden and severe pain in the knee joint. The cause of the necrosis is largely unknown, although the surgeons suspect a damage to the blood circulation in the bone.
The necrotic lesion is limited to only one femoral condyle in only one knee.
The X-ray picture shows initially no changes. As the disease progresses, there develops flattening of the joint surface of the femoral condyle and there appears sclerosis of the bone under the joint surface.
The MRI examination of the knee joint usually discovers the changes already in the early stages, when the X-ray picture is still normal. (Also the bone scan is positive in the early stages of the disease)
Atraumatic osteonecrosis
involves large areas of the knee joint and is associated with specific risk factors such as use of corticosteroid drugs or abuse of alcohol.
The knee is the second most common joint suffering from osteonecrosis and is affected about five times less often than the hip joint.
The consequences of the necrosis of the femoral condyle depend on the size of the necrotic lesion. Small size lesions heal without damage to the knee joint, large lesions progress quickly to osteoarthritis of the knee joint.
The treatment of the necrosis of the femoral condyle depends on the size of the lesion. Patients with small lesions are usually treated with unloading of the knee (crutches, braces). Some surgeon treat these patients with osteotomy. For lesions affecting large areas of the knee there are few treatment options other than total knee arthroplasty
The previously infected knee.
Some patients who as children have had bacterial knee joint infection, develop later painful secondary osteoarthritis of the knee joint . These patients are candidates for total knee replacement if
- the infection is healed several years clinically (no drainage or swelling of the knee joint area)
- blood test show no signs of infection activity
- X-ray pictures show no areas of chronic bone infection (osteomyelitis).
Still, the original infection is never healed, it is only sleeping and it can be awaken to life by the total knee surgery.
The results of TKR after previous infection depend on the bacteria that caused the original joint infection.
The lowest rates of recurrence of the original infection (less than 10 %) have patients whose knee joint infection was caused by Gram-positive bacteria, followed by patients with “healed” tuberculous infection. The worst results, with recurrence of infection in more than 20%, have patients with joint infection caused by Gram-negative bacteria.
(Gram-positive and Gram-negative refers to the staining properties of bacteria discovered by the Danish bacteriologist H. C. Gram)
The risks with operation of a previously infected knee joint:
The surgeon may discover a core of active bone infection during the operation, containing pus and rests of necrotic bone. Most surgeons will not continue with the operation in this case. They will take away all infected tissues, put a drain in the knee joint and perhaps also chunks of bone cement with antibiotics into the wound and start leg traction. Alternative is a spacer, formed as a future total knee and fabricated from bone cement saturated with antibiotics. Leg traction is then not necessary.
The patient will also receive large doses of antibiotics.This treatment may take months, the patient will be most time on crutches. First when this infection has healed the surgeon can contemplate a new attempt at total knee replacement
The original infection may flare up after total knee replacement. To prevent this complication, the patients are usually put on a long regime of antibiotics, sometimes life-long.
There is a risk connected with long-term antibiotics treatment: It may produce successively antibiotics-resistant bacteria; and it may produce side-effects in the patients, many of them may be serious or even lethal (necrotising bowel inflammation).
The function in the muscles around the stiff knee is usually difficult to assess before the operation. After the operation, with the knee joint now mobile, it may appear that the muscles have low strength. This muscle insufficiency may cause limp and joint instability.